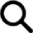How Pain and Depression Create a Vicious Cycle
|
Reading time: 8 minutes
|
Key Takeaways
- Long-term pain can affect mood, while depression can make pain feel worse. Many people experience both conditions at the same time, creating a cycle that impacts daily life and emotional well-being.
- Managing pain and depression at the same time can improve overall well-being. Treatment may include therapy, physical rehabilitation, and medications that support both mood and pain relief, such as SSRIs (Prozac), SNRIs (Effexor), or NDRIs (Wellbutrin).
- Doctors, therapists, and pain specialists can create treatment plans based on individual needs. Cognitive Behavioral Therapy (CBT), physical therapy, lifestyle changes, and medication management can provide relief.
Pain and mental health are closely connected, affecting both the body and emotions. Chronic pain and depression often occur together, making daily activities harder and lowering overall well-being. When pain lasts for weeks or months, it can impact mood, drain energy, and take away enjoyment from life. At the same time, depression can make the body more sensitive to pain, causing discomfort to feel stronger than it actually is.
Research shows a strong link between these conditions. About 20% of adults experience chronic pain, while 8.1% deal with major depression at any time. Many people struggle with both, creating a cycle where pain leads to sadness and stress, and emotional distress makes pain worse.
Understanding how chronic pain and depression affect each other helps people find better ways to manage their health. Treating both conditions together with mental health medications, therapy, and lifestyle changes can improve daily life, bring emotional balance, and reduce discomfort. Whether pain triggers depression or depression makes pain harder to handle, recognizing this connection allows individuals and healthcare providers to create effective treatment plans.
What Is Chronic Pain?
Chronic pain is long-lasting discomfort that continues for 12 weeks or more, even after an injury heals or a health condition is treated. Unlike short-term pain that goes away with recovery, chronic pain persists and can affect movement, mood, and daily activities.
What Causes Chronic Pain?
The reasons for chronic pain vary from person to person. Some people develop it after an injury or surgery, while others experience it due to nerve damage or long-term health conditions. Some medical conditions that can lead to ongoing pain include:
- Arthritis – Joint inflammation that causes stiffness and discomfort
- Endometriosis – A condition where tissue similar to the lining of the uterus grows outside the womb, leading to pain
- Temporomandibular Joint (TMJ) Disorder – A problem with the jaw joint that causes pain in the face, head, and neck
In some cases, doctors cannot pinpoint the exact cause, making treatment more challenging.
How Chronic Pain Feels
People experience chronic pain in different ways, and the level of discomfort can change over time. Common sensations include:
- A dull, ongoing ache that never completely goes away
- Sharp or burning pain that appears suddenly and unexpectedly
- Muscle tightness and stiffness that limit movement and flexibility
Who Is at Higher Risk?
Anyone can develop chronic pain, but some people are more likely to experience it:
- Older adults – The body’s ability to heal slows down with age, increasing the risk of long-term pain
- People recovering from injuries or surgeries – Damaged muscles, nerves, or bones may continue to cause discomfort after healing
- Individuals with chronic illnesses – Conditions like diabetes, fibromyalgia, or nerve disorders can lead to ongoing pain
Recognizing chronic pain early allows individuals to seek treatment and support. Managing pain effectively can improve daily life, help maintain physical health, and reduce emotional distress.
Can Depression Cause Physical Pain?
Depression affects more than just emotions—it can also cause physical discomfort that interferes with daily life. Depression has been linked to muscle tension, nerve sensitivity, and changes in brain chemistry, which may lead to physical symptoms such as: muscle stiffness, headaches, and digestive issues.”
How Depression Affects the Body
Many physical symptoms of depression are linked to muscle tension, nerve sensitivity, and changes in brain chemistry. Common effects include:
- Muscle stiffness and joint pain, especially in the back, shoulders, and lower back
- Tension headaches that start occasionally but become more frequent or severe over time
- Digestive issues, such as stomach pain, nausea, or irregular bowel movements
Why Does Depression Cause Pain?
The connection between depression and pain is rooted in chemical imbalances within the brain. Neurotransmitters such as serotonin and dopamine help regulate both mood and pain perception. When their levels drop, the brain processes pain signals differently, making discomfort feel more intense than usual. Lower serotonin levels can also contribute to increased inflammation, which may worsen muscle and joint pain.
Managing Depression-Related Pain
Addressing both depression and physical discomfort can lead to relief. Treatments such as therapy, lifestyle changes, and medication may help restore balance in the brain and improve overall well-being.
Some people find relief with SSRIs (e.g., Prozac) and SNRIs (e.g., Effexor), which help regulate serotonin levels. These medications are commonly prescribed to manage depression and may also reduce physical symptoms associated with mood disorders.
Can Chronic Pain Lead to Depression?
Chronic pain affects more than just the body—it can also impact emotions, motivation, and daily life. Living with long-term pain can lead to changes in mood and behavior, sometimes resulting in depression. When pain does not go away, it can make once-enjoyable activities feel frustrating or impossible.
How Chronic Pain Affects Mental Health
Pain that lasts for weeks or months can make even simple tasks feel tiring. Over time, this can lead to:
- Irritability, fatigue, and sadness, making it harder to stay involved in daily activities
- Loss of interest in hobbies and social connections, leading to isolation
- Difficulty exercising, which lowers endorphin levels—natural chemicals that help boost mood
The Pain-Depression Cycle
Chronic pain and depression often affect each other, creating a difficult cycle:
- Pain lowers mood, making it harder to feel motivated
- Depression reduces pain tolerance, making discomfort feel worse
- Pain increases, leading to frustration and emotional distress
- Mood declines further, making pain management even more challenging
Without the right support, this cycle can continue, making it harder to recover.
Managing Pain and Depression Together
Addressing both physical pain and emotional distress can improve daily well-being. Treatment may include therapy, physical rehabilitation, lifestyle changes, or medication to help balance mood and reduce discomfort.
Some people find relief with NDRIs (e.g., Wellbutrin), which help regulate norepinephrine and dopamine—two neurotransmitters that influence mood and pain perception. Restoring these chemical levels can improve energy and reduce the emotional toll of chronic pain.
How to Manage Both Chronic Pain and Depression
Chronic pain and depression are often connected, and treating both can improve daily life. Whether depression makes pain feel worse or pain leads to emotional distress, finding the right approach can help. A combination of medical support, therapy, and lifestyle changes often works best.
Seeking Medical Support
Doctors and specialists can help create a treatment plan based on individual needs:
- If depression is the main concern, a psychiatrist or therapist may suggest counseling, lifestyle changes, or medications to support mental health.
- If pain is the bigger issue, a general practitioner (GP) or pain specialist might recommend physical therapy, pain relief strategies, or a referral to a mental health professional for additional care.
Treatment Approaches
1. Therapy & Lifestyle Changes
Some habits and therapies may improve both pain and mood:
- Cognitive Behavioral Therapy (CBT) – Teaches coping strategies for managing emotional distress and pain perception.
- Exercise – Boosts endorphins, which help reduce pain and improve mood.
- Better Sleep Habits – Getting enough rest helps the body heal and supports emotional balance.
2. Medication Options
Some medications can help with both mental health and pain symptoms:
- SSRIs (e.g., Prozac) – Help regulate serotonin levels, which may improve mood and reduce sensitivity to pain.
- SNRIs (e.g., Effexor) – Increase serotonin and norepinephrine, supporting nerve-related pain relief and emotional stability.
- NDRIs (e.g., Wellbutrin) – Help balance dopamine levels, which may improve energy levels and reduce pain-related mood changes.
3. Physical Pain Treatments
- Physical Therapy – Strengthens muscles, improves mobility, and reduces strain on painful areas.
- Medication Adjustments – Some antidepressants also help manage pain, so a doctor may adjust prescriptions for better results.
- Alternative Treatments – Acupuncture, massage therapy, and relaxation techniques may provide additional relief.
If a doctor recommends medication for chronic pain or depression, affordable options may be available through a trusted online Canadian pharmacy.
Addressing both physical pain and emotional well-being can improve quality of life, allowing individuals to regain control and feel more like themselves again.
Final Thoughts
Dealing with chronic pain and depression can feel overwhelming, especially when symptoms last for weeks or months. Since these conditions affect each other, recovery can be more challenging without proper support. Recognizing when to seek help is an important step toward feeling better and improving daily life.
Breaking the Pain-Depression Cycle
Long-term pain can lower mood, while depression can make pain feel worse. Treating both conditions together can lead to better symptom relief and a higher quality of life. Early support from doctors, therapists, and lifestyle adjustments can help prevent symptoms from getting worse.
Support Options
- Medical Professionals – Doctors, psychiatrists, and therapists can assess symptoms and create a treatment plan that fits individual needs.
- Therapeutic Approaches – Cognitive Behavioral Therapy (CBT), relaxation techniques, and physical therapy may help with both pain and emotional distress.
- Medication Management – If prescribed, antidepressants or pain-relief medications can help balance serotonin, norepinephrine, and dopamine levels, which support both mood and pain relief.
If a healthcare provider recommends medication, ordering from a licensed Canadian online pharmacy can offer a convenient way to access treatment from home.
Getting the right support can make a difference. With professional care and a personalized plan, individuals can find relief from both physical pain and emotional struggles, making it easier to regain control over daily life.
Information provided on this website is for general purposes only. It is not intended to take the place of advice from your practitioner